Photo: Research Matters
Can you imagine being so hungry that you have to eat your own parts? Sound gruesome, is it not? But guess what? We have all been there and done that, and that too, not once, but many times! And how? Blame it on our cells, which have the ability of “autophagy”.
When living cells experience a severe shortage in nutrient supply, they often devour or deconstruct unnecessary and dysfunctional components to generate the amino acids and nutrients needed to produce energy and perform basic functions. This well regulated, self-eating process is called “autophagy”. Studies have shown that autophagy not only helps cells survive periods of starvation, but also maintains cellular equilibrium - both of which are essential for survival and normal functioning of cells. This process also plays an important role in immune response and controls inflammation and activation of adaptive immunity.
“Autophagy is essential for survival of the organism because it keeps the cells and organism healthy by removing damaged organelles and aggregated and misfolded proteins, fighting infections and preventing cancer. Defects in autophagy lead to several prevalent disorders including cancer, neurodegenerative diseases and hampered immune response. Because autophagy has direct relevance to human health and disease, it is necessary to understand the molecular mechanisms underlying this vital process,” says Dr. Ghansyam Swarup, a molecular biologist based at the Centre for Cellular and Molecular Biology, Hyderabad, stressing on the need for understanding this complex process. Today, autophagy is an important field of research in cell biology and the fact that the 2016 Nobel Prize in Physiology was awarded to the Japanese cell biologist Prof. Yoshinori Ohsumi, is a testimony to this.
Tracing the trails of Autophagy
The interest on autophagy started with the discovery of lysosome, a cell organelle that contains enzymes that can break down all the biomolecules, by Christian de Duve in 1955. Following that, many studies employed electron microscopy to observe lysosome and established that the degradation of foreign particles takes place inside them. The vesicle, which carries foreign bodies to lysosome, was termed phagosome. Further studies discovered similar membrane structures containing cellular organelles like mitochondria and other cytoplasmic constituents. These double membrane-bound structures, which could be induced by certain chemical treatments or stress conditions, were shown to fuse with lysosome. The term 'autophagy’, literally meaning ‘self-eating’, was coined to refer to this mode of delivery of cytoplasmic materials to lysosome for degradation. The lack of sophisticated instruments and unavailability of biomarkers limited further studies in this area during the 1970s and 1980s. The real breakthrough came in 1993 when Dr. Ohsumi and his colleagues isolated 15-autophagy deficient mutants in yeast, thus unravelling the genetics behind 'autophagy'.
“Prof. Ohsumi first established that autophagy occurs in yeast. This required development of a yeast strain deficient in three lysosomal enzymes, which accumulated non-degraded material in its lysosome when autophagy was induced using nutrient-deficient medium and could be seen under a light microscope. Using this yeast strain, he could identify and isolate autophagy-defective mutants because they did not accumulate non-degraded material in the vacuole. Subsequent cloning of these genes led to identification of molecular markers for the study of autophagy in yeast. Since most of these autophagy genes are also present in mammalian cells, his work helped in exploring autophagy mechanisms even in mammalian cells”, explains Dr. Swarup, who recently published his commentary on the Nobel winning research.
Autophagy is generally classified into three types owing to differences in the underlying mechanism; macroautophagy, microautophagy and chaperone-mediated autophagy. During earlier days of research, only macroautophagy was known and the term autophagy was used to refer to macroautophagy. It is the commonest of the three and begins with the appearance of a small membrane sac (the phagophore or isolation membrane) in the cytoplasm, which then extends into a double membrane-bound structure enclosing a portion of the cytoplasm. This double membrane-bound structure, called autophagosome, then fuses with lysosome, where actual degradation and recycling takes place. In microautophagy, autophagosomes or similar structures are not involved and the lysosome engulfs the constituents to be degraded directly from the cytoplasm. In the case of chaperone-mediated autophagy (CMA), as the name suggests, the autophagy is dependent on protein-complexes called chaperones that deliver cargo to be degraded, into the lysosome.
Autophagy and its importance
Though autophagy is a necessary process in our cells, the multi-step nature of autophagy makes it vulnerable to failure at different levels. Studies have shown that autophagy is critical to maintaining cellular equilibrium and hence, it becomes all the more important in cells with longer life span, like neurons. It is no coincidence that defects in autophagy have been linked to neurodegenerative diseases like Parkinson’s disease, Alzheimer’s disease, Huntington’s disease, ALS and glaucoma. Alterations in autophagy are also observed in cells affected by cancer, metabolic dysfunction, vascular instability, cardiomyopathies, myopathies and non-alcoholic fatty liver disease (Crohn's disease). Researchers are trying to develop drugs that can either induce or inhibit autophagy and studies are also being carried out to repurpose known drugs, which are reported to enhance or inhibit autophagy, for new clinical applications.
But, to effectively use drug induced inhibition or enhancement of autophagy as a therapeutic measure, we need to identify the step(s) affected in causing these diseases. Prof. Ohsumi's identification of autophagy related genes in yeast was definitely a turning point in this direction. The hallmarks of this study are design of elegant methodologies, which could be extended to higher animals and near-complete description of autophagy in a model organism like yeast. When read in the context of therapeutic promises autophagy offers, it is no wonder that Prof. Oshumi was awarded the Nobel Prize.
Research trends in Autophagy
Despite the enormous volume of work over the past two to three decades, autophagy research is still in its early stages. To quote Prof. Oshumi from a review published in 2014:
“There are so many questions that remain to be answered about the unique membrane dynamics that constitute autophagy, and there are still a great deal of mysteries to be uncovered before we truly understand the molecular mechanisms of autophagy.”
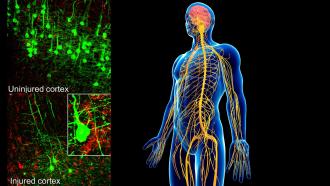
Autophagy research is an active area in India too. “Several groups in India are actively working to understand molecular mechanisms of autophagy and its role in various diseases at several institutions. They are using a variety of experimental models including cell culture and animal models, and pathogens such as malarial parasite and Leishmania donovani”, remarks Dr. Swarup, whose lab is actively investigating the role of the protein ‘optineurin’, in autophagy and other cellular functions. The mutations in optineurin are reported to cause both glaucoma and ALS (Amyotrophic Lateral Sclerosis) - a fatal, progressive disease, which involves degeneration of motor neurons of the primary cortex, brainstem and spinal cord. Dr. Swarup's work has shown that glaucoma-associated mutants of optineurin impair autophagy, vesicle trafficking and signalling.
Understanding connections between autophagy and human diseases, characterisation of genetics of autophagy in other organisms and the role of autophagy in immune responses are some of the themes being explored by various research groups across the globe. With further advancements in analytical techniques, we would hopefully be able to tap into the enormous potential of the self-snacking abilities of cells – ‘autophagy’.